News headlines are screaming about class action lawsuits being filed against drug companies selling the oral form of a nasal decongestant that the FDA says doesn’t work. It’s called phenylephrine. Phenylephrine has been around since the early 1970s and it’s a common ingredient in over-the-counter (OTC) cold remedies found in grocery stores in the medicine aisle.
The FDA advisory committee met on September 11-12, 2023 about phenylephrine-containing oral products and there is a clarification of the FDA committee’s decision to identify them as ineffective that was posted on September 14, 2023.
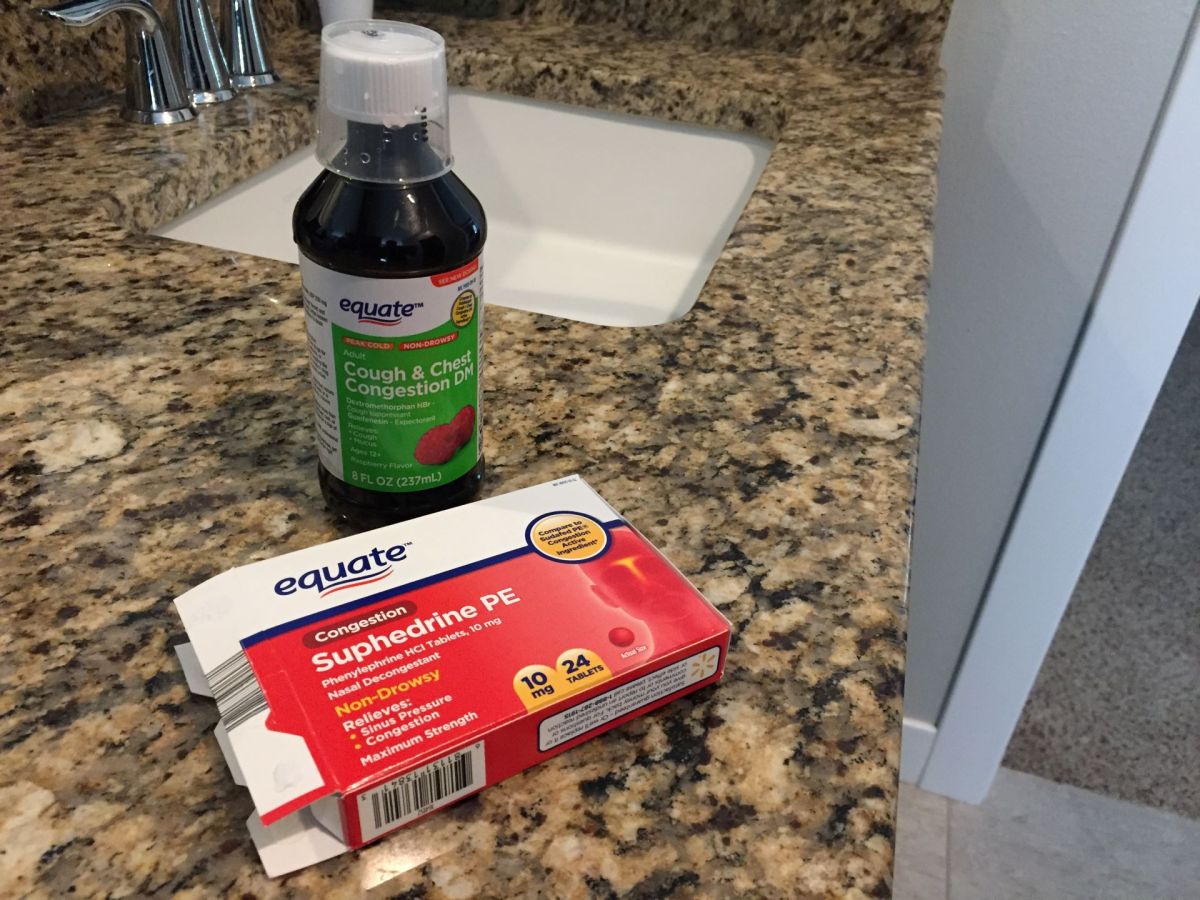
A common OTC containing the agent is Sudafed PE. The Equate version of it is Suphedrine PE, which is cheaper. The name capitalizes on its similarity to the name Sudafed, which is pseudoephedrine—which is an effective oral agent for relieving nasal congestion. The problem with it is that it’s been behind-the-counter since 2006 because it can be used in the manufacture of methamphetamine.
Sena bought a box of Suphedrine PE the other day because she caught a head cold. She thinks it’s helplful.
I took a quick look at a few of the presentations of the FDA Advisory Committee meeting. Mainly I just noted the last slide of the FDA presentation, which said that recent studies showed phenylephrine 10 mg was not significantly different from placebo.
Another presentation showed that a large consumer survey indicated that Americans rely on phenylephrine and thought it was an effective nasal decongestant.
This reminded me of Serutan, which is just Nature’s spelled backwards. Serutan was not a placebo; it was a fiber-based laxative, but a lot of people made fun of it. But that, in turn, reminded me of Geritol, which was sold as a tonic a long time ago and which, for a while, was thought by many people to help women get pregnant. Who knows? Maybe some people still believe that, although even the manufacturer disputes the claim.
On the other hand, this in turn reminded me of a medication called Obecalp. You can find many web entries about Obecalp, which is just “placebo” spelled backwards. Some physicians may still be prescribing Obecalp (placebos don’t always have to be pills). In general, the opinion about the ethics of the practice is expressed in a recent paper (Linde K, Atmann O, Meissner K, Schneider A, Meister R, Kriston L, Werner C. How often do general practitioners use placebos and non-specific interventions? Systematic review and meta-analysis of surveys. PLoS One. 2018 Aug 24;13(8):e0202211. doi: 10.1371/journal.pone.0202211. PMID: 30142199; PMCID: PMC6108457.):
“Although the use of placebo interventions outside clinical trials without full informed consent is generally considered unethical [1–3], surveys in various countries show that many physicians prescribe “placebos” in routine clinical practice [4–7].”
There’s actually a fairly large body of research about placebo effects. One really long paper has interesting conclusions and key points (Wager TD, Atlas LY. The neuroscience of placebo effects: connecting context, learning and health. Nat Rev Neurosci. 2015 Jul;16(7):403-18. doi: 10.1038/nrn3976. PMID: 26087681; PMCID: PMC6013051.):
Conclusions:
A substantial part of the therapeutic benefit patients experience when undergoing medical treatment is caused by their brain’s response to the treatment context. Laboratory investigations of placebo effects provide a way of examining the brain mechanisms underlying these effects. Consistent findings across studies include reduced activity in brain areas associated with pain and negative emotion, and increased activity in fronto–striatal–brainstem circuits. In most cases, the creation of robust placebo effects across disorders and outcomes seems to require appropriate conceptual beliefs — maintained in prefrontal cortical networks — that are supported by experience-dependent learning in striatal and brainstem circuits. However, the critical ingredients for eliciting placebo effects, at both the psychological and brain level, are just beginning to be understood. These ingredients may differ substantially depending on whether the outcomes are symptoms, behaviours or changes in physiology. A better understanding of the neuroscience of placebo could yield rich benefits for both neuroscience and human health.
Key Points:
- Placebo effects are effects of the context surrounding medical treatment. They can have meaningfully large impacts on clinical, physiological and brain outcomes.
- Effects of placebo treatments are consistent across studies from different laboratories. These effects include reduced activity in brain areas associated with pain and negative emotion, and increased activity in the lateral and medial prefrontal cortex, ventral striatum and brainstem.
- Placebo effects in pain, Parkinson disease, depression and emotion are enabled by engagement of common prefrontal–subcortical motivational systems, but the similarity across domains in the way these systems are engaged has not been directly tested.
- Meaningfully large placebo effects are likely to require a mixture of both conceptual belief in the placebo and prior experiences of treatment benefit, which engage brain learning processes.
- In some cases, placebo effects are self-reinforcing, suggesting that they change symptoms in a way that precludes extinction. The mechanisms that drive these effects remain to be uncovered, but doing so could have profound translational implications.
I will probably catch Sena’s head cold. By the way, Phenylephrine spelled backwards is enirhpelynehp.