Here’s a redux of one of my blog posts from years ago. There’s not been much change in the data or clinical practice regarding delirium, except we’re even less enthusiastic about using any kind of psychotropic medication to treat delirium, even hypoactive delirium. Try the puzzle.
“So, you want to put on a game show contest to educate clinicians about delirium? Contact David Meagher, a psychiatrist in (where else?) Limerick, Ireland. He reported on this innovative educational workshop in the November 2010 Vol. 3 issue of the Annals of Delirium, the newsletter for the European Delirium Association (EDA). He also published the study which describes the contest in International Psychogeriatrics [1].
The workshop focused on clinician attitudes toward drug therapy for distressed delirious patients. It explored pre-existing attitudes and practice toward the use of medications to manage delirium and exposed participants to a very interactive educational event modeled after a popular TV quiz show. There were two teams (skeptics versus neuroleptics) furnished with a list of statements about delirium pharmacotherapy. The participants later completed a post-workshop questionnaire that explored changes in attitudes as a result of the workshop.
The participants were all experts on the subject and there was a good deal of variability in attitudes and practice. Some of the questions put to the teams involved using antipsychotics prophylactically to prevent delirium, the mechanism of action of antipsychotics, and what role benzodiazepines play in the treatment of non-alcohol withdrawal delirium.
One of the more puzzling findings was that the frequency of antipsychotic use was inversely proportional to the perception of the strength of supporting evidence. In other words, the less they knew about antipsychotics, the more often they used them. Most participants seemed to believe that the principal mechanism of action of antipsychotics is sedation, despite the lack of supporting evidence.
Some clinicians used antipsychotics to relieve the stress of caregivers rather than that of delirious patients, an example of patients getting the right treatment for the wrong reasons as observed by Meagher—and many of us in the field.
The workshop also highlighted the tendency of clinicians to focus on risk management rather than effective therapeutic intervention in the management of delirious patients with disruptive behavior and severe distress. This mainly relates to focus on the potential adverse effects of antipsychotics such as extrapyramidal side effects, metabolic, and cerebrovascular effects.
The quiz show activity was fun and challenging. The device of dividing the participants into two small teams with larger audience participation cut down on the anxiety that could be provoked by giving the “wrong answer”. The questions were true/false and didn’t always have clear right or wrong answers. It was highly interactive, a component of continuing medical educational (CME) activities that is increasingly encouraged because it’s more likely to lead to changes in clinician attitude and practice. The one time Grand Rounds CME “seat time” is going the way of the dinosaur.
So a couple of findings from the quiz show post-activity questionnaire were that clinicians were more likely to use antipsychotics prophylactically and to use antipsychotics to manage hypoactive delirium.
Our delirium intervention project group members are not quite as enthusiastic yet about these two interventions. We’re a bit more inclined at least initially to focus on non-pharmacologic multicomponent strategies such as the example below:
- Minimize the use of immobilizing catheters, intravenous lines, and physical restraints
- Avoid immobility, early mobilization
- Monitor nutrition
- Provide visual and hearing aids
- Monitor closely for dehydration
- Control pain
- Monitor fluid-electrolyte balance
- Monitor bowel and bladder functioning
- Review medications
- Reorient communications with the patient
- Place an orientation board, clock, or familiar objects (i.e., family photographs) in patient rooms
- Encourage cognitively stimulating activities such as word puzzles
- Facilitate sleep hygiene measures, including relaxation music or tapes at bedtime, warm drinks, and gentle massage
- Minimize noise and interventions at bedtime, e.g., by rescheduling medication times
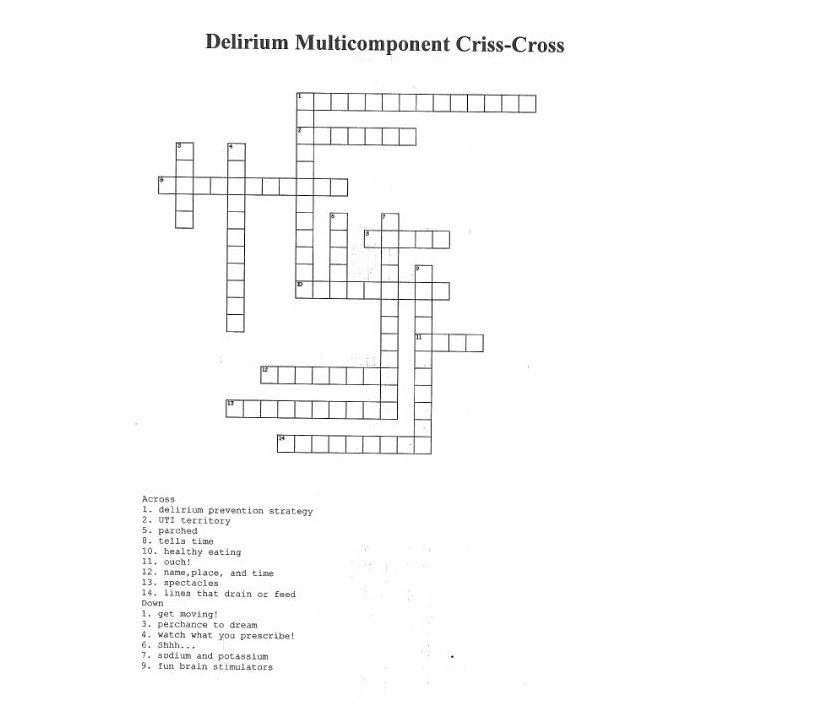
But I’m just as enthusiastic about interactive educational methods to engage learners in order to build a culture more likely to produce champions who will lead the delirium prevention effort—try the delirium multicomponent crisscross puzzle below. The clues are contained in the list of multicomponent tactics above.”
- Meagher, D.J., Impact of an educational workshop upon attitudes towards pharmacotherapy for delirium. Int Psychogeriatr, 2010. 22(6): p. 938-46.




